My mom would unwrap the white butcher paper and peel back the plastic wrap before in two quick motions that were almost natural after years of cooking. The fresh sausage would hit the skillet with a sizzle, the fat melting quickly and drops of grease flying above the black cast iron surface.
Growing up, I didn't know any other way. Gravy made with sausage ground that week at the butcher and cooked in a cast iron skillet.
I didn't know about stainless steel or copper, T-Fal or anodized, ceramic or aluminum. It was cast iron that you cooked with. But as I grew older, I equated the cast iron with my lower middle class upbringing and opted for cookware that seemed more modern, trendy.
Then as I grew older still, I found myself wishing for the heavy, sturdy skillets that not only felt nostalgic but imparted so much flavor to the foods I grew up eating. I would gaze at the cast iron in the store, thinking of buying a skillet or two but never finding a good enough reason to get one.
But, recently I did – per my doctor's orders.
The recommendation to cook with cast iron came from my new general practitioner and was among several to address the results of my InsideTracker test. I had the blood panel done, thanks to a partnership between Nuun and InsideTracker, in early September. The tests measured biomarkers important to performance and overall health.
When I took the test, I expected to hear that my vitamin D was low (as it had been during my pregnancy with Silas) but I felt that I was in overall good health. I was eating well, keeping up with most of the healthy habits I established during Whole30, and was at my lowest post-Si weight.
My vitamin D, though, wasn't the problem. Or at least the most pressing one – and there were some pressing issues.
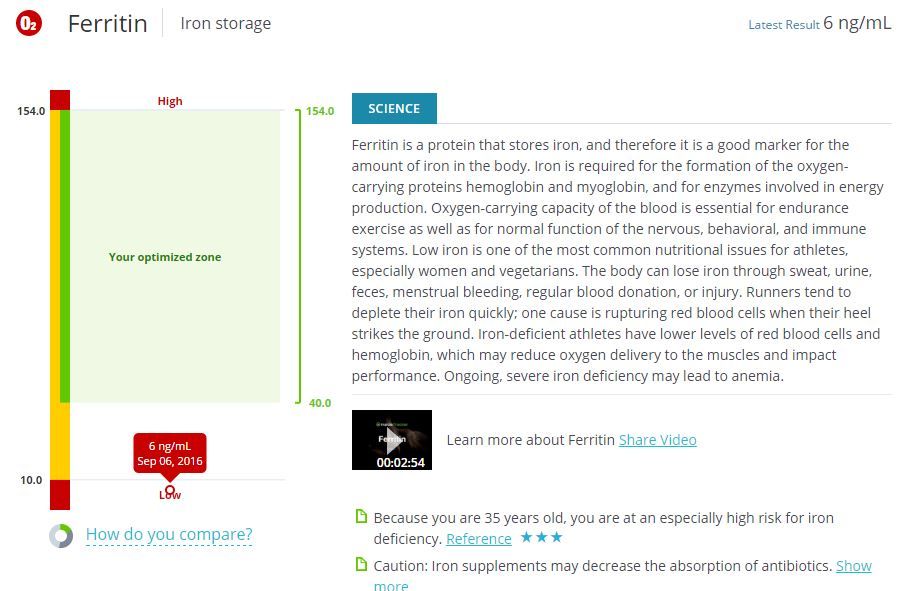
• My ferritin level was 6 ng/ml and a normal level is 11 to 307 ng/ml. According to InsideTracker, 57 percent of those tested have optimized ferritin levels and I was among the 3 percent with a low level. Ferritin is a protein that stores iron, and iron impacts the oxygen-carrying capabilities of the blood. According to the results, my iron stores are at 11 percent and my doctor said the number should at least be 20 percent. My hemoglobin levels are on the very low end level of normal but considered below the optimum level by InsideTracker for my needs and goals.
• My white blood cell count was low, coming in at 3.4 thousand/uL; normal results are 4,500 to 11,000. The lower count could indicate inflammation or other issues. My doctor was not overly concerned about this number. However, I will admit that I did freak out for a moment and spent 10 minutes convincing myself that I had an autoimmune disorder. Nine percent of InsideTracker users have a low WBC; 74 percent have an optimized level.
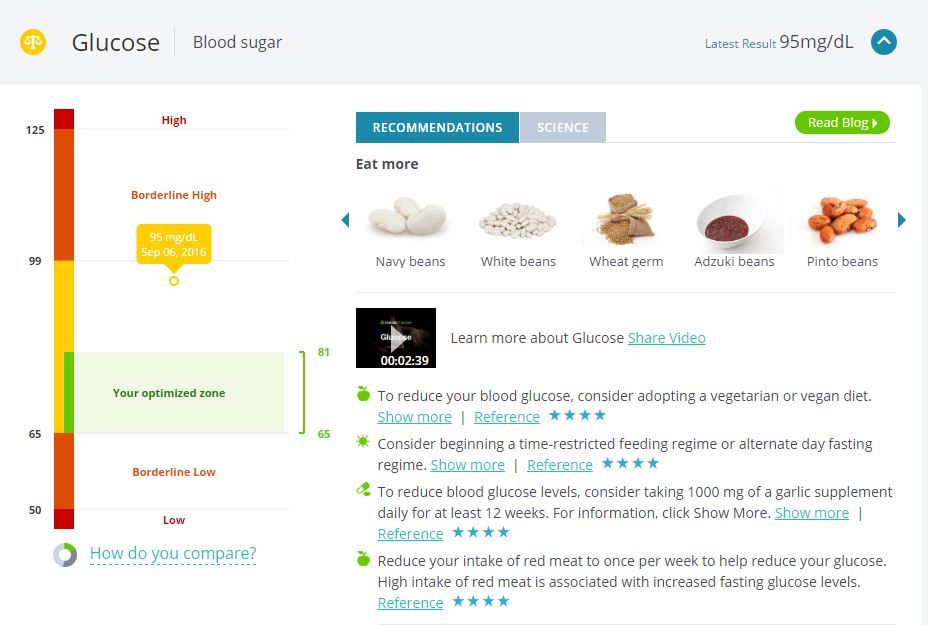
• My glucose level was 95. The InsideTracker optimized zone is 65 to 81 but my doctor said anything between 70 and 100 is OK. But 101? That is considered pre-diabetic. As someone with a strong family history of diabetes (my mom was insulin dependent and my brother is on an oral medication for the disease), my number was alarming. My doctor, whom I learned is vegan, said you are what you eat. If I am not diligent about managing my sugar cravings, I could very well put myself in a place that I have been trying to avoid: on the same track as my mom.
• While InsideTracker did not identify the levels as problematic, my doctor said that my vitamins B12 and D could use some work.
Here's the thing about InsideTracker – they don't just tell you what's wrong but they offer suggestions how to fix it. And it's not all about taking supplements.
The dietitians at InsideTracker said that I could see improvements in most areas with diet changes. To improve my iron levels, I should incorporate dark chocolate, wheat germ, soy beans and spinach. Wheat germ, granola, chia seeds, avocado and chickpeas could help my white blood cell count. As for the glucose number, beans, wheat germ, squash, fiber cereal, chia and avocado could offer aid.
I'll admit that I was a bit hesitant to make some of the changes because some of them are so anti-Whole30. I liked the control that I had when eating Whole30, as well as the changes to the way my body looked. But I learned from the test that being tired the way I have been is not normal and it's not just because I have a temperamental toddler. If I didn't want to be tired all the time (and I mean all the time), I needed to redefine what's healthy for me right now.
So it's OK to add gluten-free oats to my breakfast rotation and eat hummus in the afternoon. A low-sugar granola isn't all that bad on top of yogurt and, well, hello, dark chocolate.
Most of my changes, though, are focused on adding a green smoothie in the morning for extra spinach, incorporating more greens into my daily eating and planning at least one meal a week that features grass-fed beef from Seven Sons Farm.
I have also started taking supplements, as advised by doctor – iron, B12 and D. I also picked up an odorless garlic supplement, which was listed among potential changes by InsideTracker. There's some evidence that garlic can help with sugar levels but it might just be for diabetics. However, as diabetes is a real hot spot for me, I will do anything that I can to lower that level.
It's hard to say whether the changes have helped. It can take time to build up iron stores – my doctor anticipates that I'll take the supplements for six months – and we've had a string of rough nights thanks to teething. However, I feel good knowing where my health really stands and that I'm doing something to improve it.



Isn't that another proof that eliminating food groups from your diet is the wrong thing to do? I was never a friend of WHOLE30, Paleo, Atkins and such. I think that test reveals that those things are not good for you.
ReplyDeleteBut good for you that you ran that test. I hope you'll feel better in the future.